Alpha vs Beta Thalassemia explains the differences between two main types of thalassemia disorders. Alpha thalassemia affects alpha globin chain production, while beta thalassemia affects beta globin chains in hemoglobin. Both conditions are inherited blood disorders that can range from mild to severe depending on gene mutations. Understanding the difference helps in proper diagnosis, treatment planning, and genetic counseling for affected individuals and families.
Understanding Hemoglobin and Thalassemia’s Impact
To understand how thalassemia affects the body, it is important to first look at the structure of hemoglobin. Normal adult hemoglobin consists of four protein chains: two alpha-globin chains and two beta-globin chains. These chains must be produced in balanced amounts to form healthy red blood cells that efficiently carry oxygen throughout the body.
Thalassemia occurs when genetic mutations disrupt the production of these chains. In alpha vs beta thalassemia, the difference lies in which globin chain is affected. If the body cannot produce enough alpha chains or beta chains, the imbalance leads to defective red blood cells. These cells are often small, pale, and fragile, and are destroyed faster than normal cells, leading to anemia.
The condition follows an autosomal recessive inheritance pattern. This means a person develops a severe form of thalassemia only when they inherit faulty genes from both parents. If only one defective gene is inherited, the individual becomes a carrier of alpha thalassemia or beta thalassemia. Carriers are usually healthy but can pass the gene to their children, which is why understanding the difference between alpha and beta thalassemia is important for genetic counseling and family planning.
Alpha Thalassemia: A Closer Look
 Alpha thalassemia happens when the body cannot produce enough alpha-globin chains. The production of these specific chains is controlled by four genes located on chromosome 16. You inherit two of these alpha-globin genes from your mother and two from your father. Unlike many other genetic conditions caused by gene mutations, alpha thalassemia is almost always caused by gene deletions—meaning the genes are entirely missing from the DNA sequence.
Alpha thalassemia happens when the body cannot produce enough alpha-globin chains. The production of these specific chains is controlled by four genes located on chromosome 16. You inherit two of these alpha-globin genes from your mother and two from your father. Unlike many other genetic conditions caused by gene mutations, alpha thalassemia is almost always caused by gene deletions—meaning the genes are entirely missing from the DNA sequence.
The severity of alpha thalassemia is directly linked to the number of missing genes. The condition is broken down into four main forms:
Silent Carrier State
When only one of the four alpha-globin genes is missing, the person is considered a silent carrier. The three remaining functional genes produce enough alpha-globin to keep hemoglobin levels completely normal. Silent carriers experience no symptoms and usually only discover their status through targeted genetic testing.
Alpha Thalassemia Trait (Minor)
When two alpha-globin genes are missing, the diagnosis is alpha thalassemia minor. Individuals with this trait might have slightly smaller red blood cells and may experience very mild anemia. However, they generally feel healthy, require no medical treatment, and live normal, active lives.
Hemoglobin H Disease
If three alpha-globin genes are missing, a person develops Hemoglobin H disease. With only one working gene, the body faces a severe shortage of alpha chains. The excess beta chains clump together to form abnormal clusters called Hemoglobin H. These clusters damage the red blood cells, leading to moderate to severe anemia, extreme fatigue, an enlarged spleen, and bone deformities.
Hydrops Fetalis
This is the most severe form of alpha thalassemia, occurring when all four genes are missing. Without any alpha-globin, a developing fetus cannot produce normal hemoglobin to survive. Tragically, this condition usually results in miscarriage or causes the baby to pass away shortly after birth.
Diagnosis of alpha thalassemia typically begins with a standard Complete Blood Count (CBC) to check for small red blood cells. However, pinpointing the exact number of missing genes requires specialized DNA testing. Treatment for severe forms like Hemoglobin H disease involves regular monitoring, occasional blood transfusions, and medications to support healthy blood production.
Beta Thalassemia: A Deeper Dive
 Beta thalassemia occurs when the body fails to produce sufficient beta-globin chains. The genetic instructions for beta-globin are located on chromosome 11, and humans inherit just two of these genes—one from each parent. Instead of missing genes, beta thalassemia is usually caused by point mutations, which are small errors in the genetic code that severely limit or completely stop beta-globin production.
Beta thalassemia occurs when the body fails to produce sufficient beta-globin chains. The genetic instructions for beta-globin are located on chromosome 11, and humans inherit just two of these genes—one from each parent. Instead of missing genes, beta thalassemia is usually caused by point mutations, which are small errors in the genetic code that severely limit or completely stop beta-globin production.
This type of thalassemia is generally categorized into three levels of severity, depending on how the mutations affect hemoglobin output:
Beta Thalassemia Minor
When a person inherits one mutated beta-globin gene and one normal gene, they have beta thalassemia minor. The single functioning gene is usually enough to prevent serious health issues. Like its alpha counterpart, this minor trait typically causes asymptomatic or very mild anemia that does not require treatment.
Thalassemia Intermedia
If a person inherits two mutated genes, but the mutations are mild enough to allow for some beta-globin production, the result is thalassemia intermedia. The symptoms vary widely. Some individuals experience mild fatigue and bone weakness, while others face more significant anemia that requires occasional medical intervention, especially during times of illness or physical stress.
Beta Thalassemia Major (Cooley’s Anemia)
The most severe form occurs when a person inherits two severely mutated genes, resulting in little to no beta-globin production. Babies born with beta thalassemia major usually appear healthy at birth because they still rely on fetal hemoglobin. However, within the first two years of life, severe anemia sets in. Symptoms include extreme paleness, poor growth, severe bone deformities, and an enlarged liver and spleen.
Diagnosing beta thalassemia involves a CBC followed by a hemoglobin electrophoresis test, which measures the different types of hemoglobin in the blood. For those with beta thalassemia major, treatment is intensive. It requires lifelong, regular blood transfusions to maintain oxygen levels, which consequently leads to a dangerous buildup of iron in the organs.
Alpha vs Beta Thalassemia: Key Distinctions and Similarities
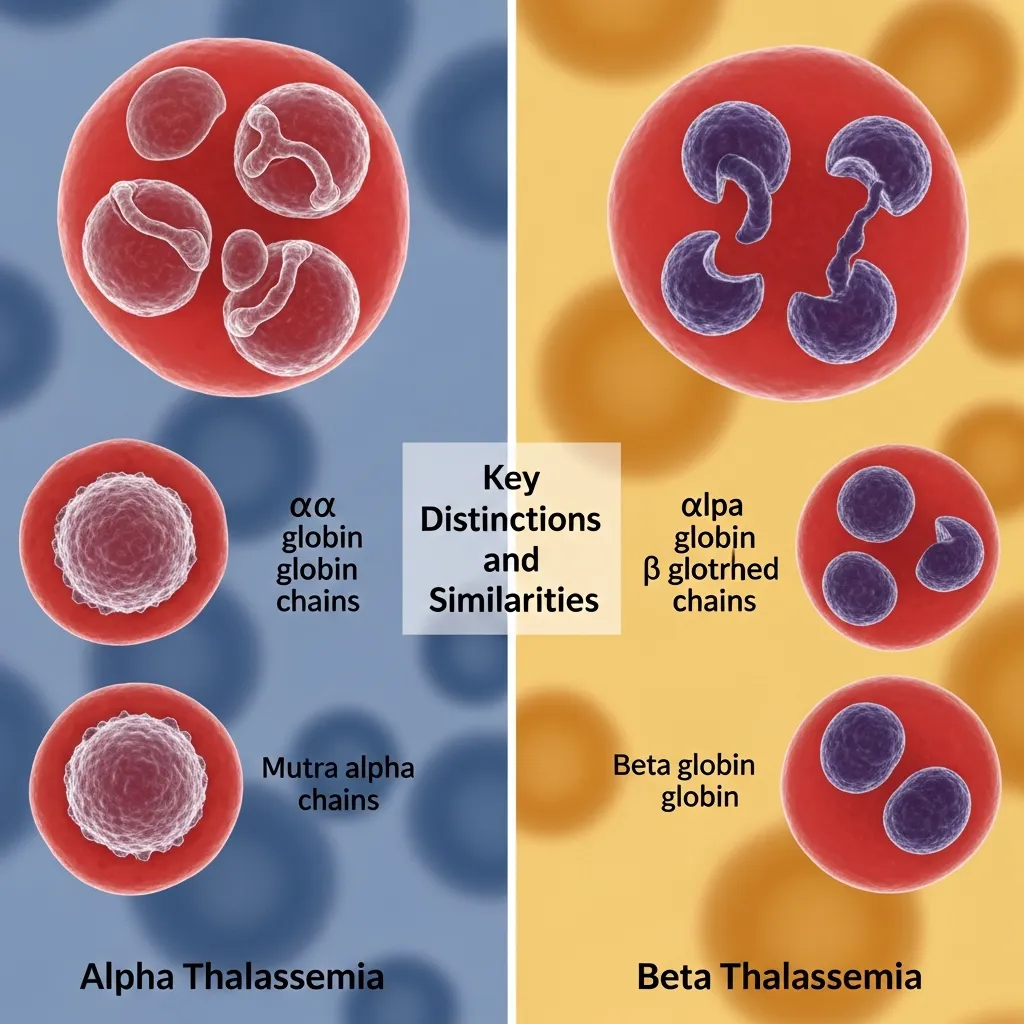 When evaluating alpha vs beta thalassemia, the most fundamental difference lies in the genetic mechanism. Alpha thalassemia involves deletion or mutation of up to four alpha-globin genes on chromosome 16, while beta thalassemia involves mutations in one or both beta-globin genes on chromosome 11. These genetic differences determine how much functional hemoglobin the body can produce and how severe the symptoms may become.
When evaluating alpha vs beta thalassemia, the most fundamental difference lies in the genetic mechanism. Alpha thalassemia involves deletion or mutation of up to four alpha-globin genes on chromosome 16, while beta thalassemia involves mutations in one or both beta-globin genes on chromosome 11. These genetic differences determine how much functional hemoglobin the body can produce and how severe the symptoms may become.
Despite these differences, both conditions share important clinical similarities. Both alpha and beta thalassemia lead to microcytic anemia, where red blood cells are smaller, paler, and less effective at carrying oxygen. In mild or “trait” forms, both conditions are usually asymptomatic and often discovered incidentally during routine blood tests. However, they are sometimes misdiagnosed as iron deficiency anemia, especially if doctors only focus on red blood cell size without further testing.
In more severe forms of alpha vs beta thalassemia, the impact on the body becomes more significant. Conditions like Hemoglobin H disease (a form of alpha thalassemia) and beta thalassemia major both result in chronic hemolytic anemia. This forces the spleen to work harder to remove damaged red blood cells, often leading to splenomegaly (enlarged spleen). Patients may experience fatigue, delayed growth, and serious complications if untreated.
Management strategies for both conditions are also quite similar. Regular blood transfusion therapy is often required in severe cases to maintain healthy hemoglobin levels. Along with transfusions, iron chelation therapy is essential to manage iron overload caused by repeated treatments. In some advanced cases, splenectomy (removal of the spleen) may be considered to reduce red blood cell destruction.
Genetic counseling plays a key role in both alpha and beta thalassemia, especially for carrier couples planning a pregnancy. Early diagnosis and proper management significantly improve quality of life and long-term outcomes for patients living with these inherited blood disorders.
Diagnosis and Genetic Counseling
Accurate diagnostic testing is the cornerstone of managing any type of thalassemia. It prevents unnecessary treatments, like the inappropriate use of iron supplements, which can cause severe organ damage in thalassemia patients.
A comprehensive diagnostic workup includes a CBC, a peripheral blood smear, and hemoglobin analysis through electrophoresis or High-Performance Liquid Chromatography (HPLC). While these tests are excellent at identifying beta thalassemia, targeted genetic DNA testing remains the gold standard, particularly for confirming silent carriers and alpha thalassemia traits.
Because thalassemia is hereditary, genetic counseling is highly recommended for carriers who are planning to start a family. A genetic counselor helps couples understand their specific gene mutations and calculates the exact risk of passing a severe form of the disease to their children. With this knowledge, families can explore prenatal diagnostic options, such as chorionic villus sampling (CVS) or amniocentesis, to make informed reproductive decisions.
Living with Thalassemia: Management and Support
Advances in modern medicine have transformed severe thalassemia from a fatal childhood disease into a manageable chronic condition. With proper care, patients with alpha vs beta thalassemia can now live into adulthood by following structured and long-term treatment plans.
The main treatment for severe cases involves regular blood transfusion therapy for thalassemia, often required every 2–4 weeks depending on the patient’s condition and hemoglobin levels. These transfusions help maintain healthy hemoglobin levels and reduce symptoms of chronic anemia.
However, repeated transfusions increase iron levels in the body, making iron chelation therapy in thalassemia essential. Chelation medications help remove excess iron and protect vital organs such as the heart and liver from damage caused by iron overload. Without proper iron management, long-term complications can become severe.
At present, bone marrow or stem cell transplantation is considered the only potential cure for thalassemia. Although it offers a chance for a permanent solution, it requires a fully matched donor and carries medical risks that must be carefully evaluated.
Lifestyle management is also an important part of thalassemia care. Patients are encouraged to maintain a balanced diet for thalassemia patients, avoid unnecessary iron supplements, and take folic acid to support red blood cell production. Regular monitoring and medical follow-up are essential for maintaining stability.
In addition to medical treatment, emotional and psychological support plays a key role in improving quality of life. Patient support groups, counseling services, and specialized healthcare centers help individuals cope with the challenges of living with a chronic blood disorder.
With proper treatment, awareness, and consistent care, individuals with alpha vs beta thalassemia can lead healthier and more stable lives despite the challenges of the conditio.
Gene therapy and genome editing, specifically CRISPR-Cas9 technology, are at the forefront of this medical revolution. Recent clinical trials have shown immense promise in editing a patient’s own hematopoietic stem cells to either correct the defective genes or stimulate the production of fetal hemoglobin, which can compensate for the defective adult hemoglobin.
Global health organizations, including the Centers for Disease Control and Prevention (CDC), continue to fund research and implement widespread screening programs. These efforts aim to improve carrier detection, educate healthcare providers, and ensure that cutting-edge therapies eventually become accessible to patients worldwide.
Looking Ahead with Hope and Knowledge
Understanding alpha vs beta thalassemia provides essential insight into how the human body produces hemoglobin and what happens when this complex system is disrupted. Although the genetic causes and biological mechanisms differ, both conditions ultimately affect red blood cell production and lead to varying degrees of anemia. For patients and families, the primary goal remains the same: achieving a healthy, stable, and fulfilling life through proper care and awareness.
Medical science continues to advance rapidly in the field of hemoglobin disorders and inherited blood diseases. Newer and safer blood transfusion therapies for thalassemia are improving patient outcomes, while modern iron chelation therapy options are helping to better control iron overload and reduce long-term complications. At the same time, ongoing research in gene therapy for thalassemia and gene-editing technologies offers hope for more permanent treatment solutions in the future.
Early and accurate diagnosis of alpha vs beta thalassemia plays a key role in effective management. Genetic testing, carrier screening, and genetic counseling help individuals understand their risks and make informed family planning decisions. These tools are especially important in preventing severe forms of thalassemia in future generations.
By combining medical treatment, regular monitoring, and informed lifestyle choices, patients can better manage symptoms and improve quality of life in thalassemia. With continued advancements in research and global awareness, there is growing hope that future treatments will reduce dependence on lifelong transfusions and bring us closer to a potential cure.
FAQs on Alpha vs Beta Thalassemia
1. What is alpha vs beta thalassemia?
Alpha vs beta thalassemia is a group of inherited blood disorders affecting hemoglobin production.
Alpha affects alpha-globin genes, beta affects beta-globin genes.
2. How are alpha and beta thalassemia different?
The main difference in alpha vs beta thalassemia is the affected globin chain.
Both cause anemia but vary in severity and symptoms.
3. Which type is more severe?
Both alpha vs beta thalassemia can be severe depending on gene mutations.
Beta thalassemia major is often more clinically severe.
4. What are common symptoms?
Alpha vs beta thalassemia symptoms include fatigue, weakness, and pale skin.
Severe cases may cause growth delay and complications.
5. Can carriers have symptoms?
Most alpha vs beta thalassemia carriers have no or mild symptoms.
They can still pass the gene to children.
6. How is it diagnosed?
Alpha vs beta thalassemia is diagnosed through blood tests and hemoglobin analysis.
Genetic testing confirms the exact type.
7. Do all patients need transfusions?
Only severe alpha vs beta thalassemia cases need regular blood transfusion therapy.
Mild cases usually do not require treatment.
8. What is iron overload?
Iron overload in alpha vs beta thalassemia happens due to repeated transfusions.
It is treated with iron chelation therapy.
9. Can lifestyle help?
Healthy lifestyle supports alpha vs beta thalassemia management.
Diet and regular monitoring improve overall health.
10. Is genetic counseling important?
Genetic counseling in alpha vs beta thalassemia helps understand inheritance risks.
It is important for prevention and family planning.
Conclusion
Alpha vs beta thalassemia are inherited blood disorders that affect hemoglobin production in different ways. Both conditions can lead to anemia and may range from mild to severe depending on genetic mutations. Early diagnosis, regular monitoring, and proper treatments like blood transfusion therapy and iron chelation therapy are essential for effective management. With genetic counseling and timely care, patients can reduce complications and maintain a better quality of life.
 Alpha thalassemia happens when the body cannot produce enough alpha-globin chains. The production of these specific chains is controlled by four genes located on chromosome 16. You inherit two of these alpha-globin genes from your mother and two from your father. Unlike many other genetic conditions caused by gene mutations, alpha thalassemia is almost always caused by gene deletions—meaning the genes are entirely missing from the DNA sequence.
Alpha thalassemia happens when the body cannot produce enough alpha-globin chains. The production of these specific chains is controlled by four genes located on chromosome 16. You inherit two of these alpha-globin genes from your mother and two from your father. Unlike many other genetic conditions caused by gene mutations, alpha thalassemia is almost always caused by gene deletions—meaning the genes are entirely missing from the DNA sequence. Beta thalassemia occurs when the body fails to produce sufficient beta-globin chains. The genetic instructions for beta-globin are located on chromosome 11, and humans inherit just two of these genes—one from each parent. Instead of missing genes, beta thalassemia is usually caused by point mutations, which are small errors in the genetic code that severely limit or completely stop beta-globin production.
Beta thalassemia occurs when the body fails to produce sufficient beta-globin chains. The genetic instructions for beta-globin are located on chromosome 11, and humans inherit just two of these genes—one from each parent. Instead of missing genes, beta thalassemia is usually caused by point mutations, which are small errors in the genetic code that severely limit or completely stop beta-globin production.


 When evaluating alpha vs beta thalassemia, the most fundamental difference lies in the genetic mechanism. Alpha thalassemia involves deletion or mutation of up to four alpha-globin genes on chromosome 16, while beta thalassemia involves mutations in one or both beta-globin genes on chromosome 11. These genetic differences determine how much functional hemoglobin the body can produce and how severe the symptoms may become.
When evaluating alpha vs beta thalassemia, the most fundamental difference lies in the genetic mechanism. Alpha thalassemia involves deletion or mutation of up to four alpha-globin genes on chromosome 16, while beta thalassemia involves mutations in one or both beta-globin genes on chromosome 11. These genetic differences determine how much functional hemoglobin the body can produce and how severe the symptoms may become.