Thalassemia is a genetic blood disorder with different types of thalassemia, including alpha thalassemia and beta thalassemia forms. Each type varies in severity from mild to severe. Understanding the types of thalassemia helps with early diagnosis, proper treatment, and better management for affected individuals and families.
The Genetic Basis of Types of Thalassemia
To understand this condition properly, it is important to look at how it is inherited. It is passed down through families in an autosomal recessive pattern, which means a child must receive altered genes from both parents to develop a severe form. If only one altered gene is inherited, the person becomes a carrier and usually shows little or no symptoms, but can still pass the gene to future generations.
Hemoglobin, the protein responsible for carrying oxygen in red blood cells, is made up of two main parts: alpha chains and beta chains. The production of these chains is controlled by specific genes in the body. Alpha chain production is linked to genes located on chromosome 16, while beta chain production is controlled by genes on chromosome 11.
When changes or deletions occur in these genes, the body is unable to produce enough normal hemoglobin. This creates an imbalance between the two types of chains, which leads to the development of different forms of the condition. In some cases, reduced alpha chain production can result in mild or more serious health effects, including Hemoglobin H disease. In other cases, problems with beta chain production can lead to similar mild or severe outcomes depending on how the genes are affected.
Understanding these genetic mechanisms is important for early detection, proper care, and prevention through medical screening and counseling. This is especially valuable in regions where the condition is more common, as awareness can help reduce the risk of severe cases in future generations.
Main Types of Thalassemia Condition
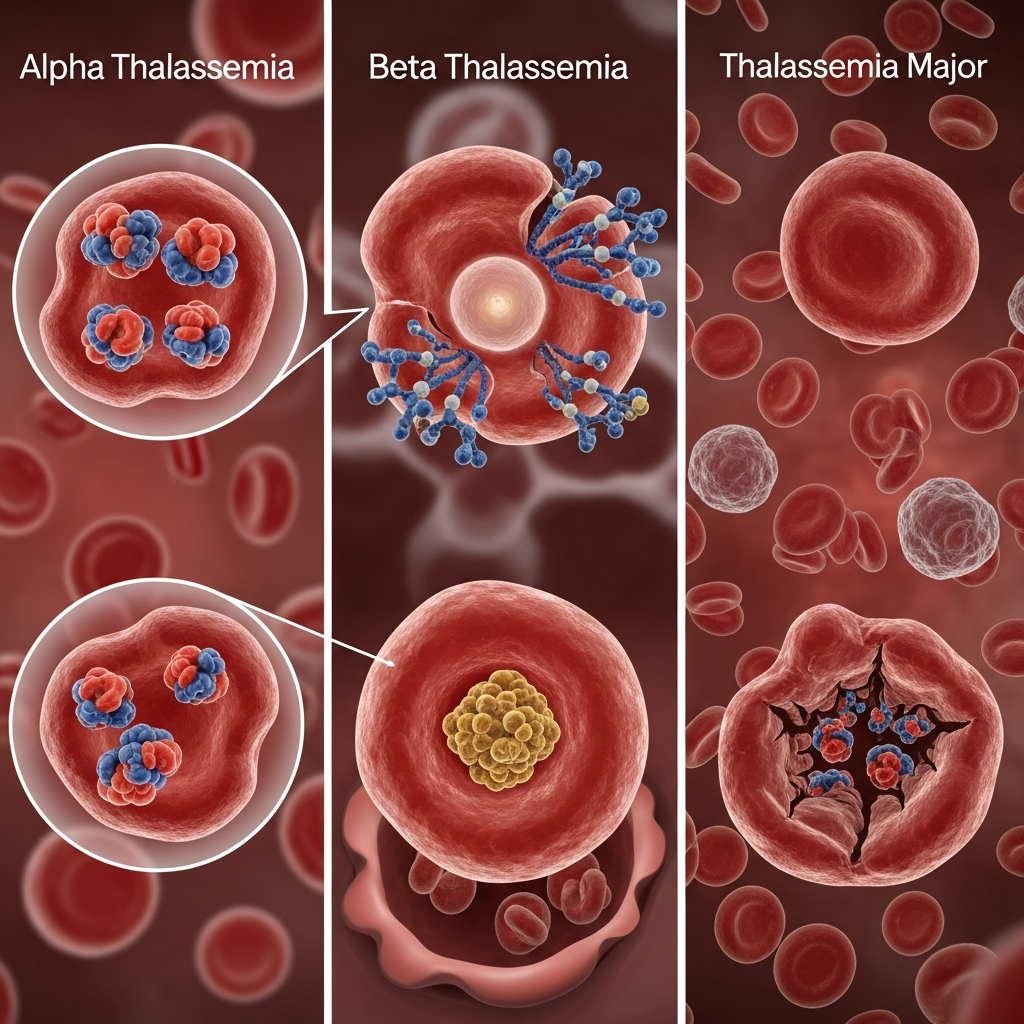 Medical professionals classify this disorder based on which part of hemoglobin is affected. The main forms arise from problems in the production of globin chains. Along with the common categories, there are also rare variations that can influence how the condition appears and how severe it becomes.
Medical professionals classify this disorder based on which part of hemoglobin is affected. The main forms arise from problems in the production of globin chains. Along with the common categories, there are also rare variations that can influence how the condition appears and how severe it becomes.
Alpha Form
This form occurs when there is a defect or missing genetic information responsible for producing alpha globin chains. A healthy person normally has four such genes, two inherited from each parent. The severity depends on how many of these genes are affected.
If only one gene is altered, the person is usually a silent carrier with no noticeable symptoms. When two genes are affected, it may cause a mild condition with slight anemia. If three genes are missing, a more serious condition develops, leading to significant anemia, fatigue, and possible complications in organs. In the most severe situation, when all four genes are missing, the condition becomes life-threatening without early medical support.
Beta Form
This form is caused by changes in the genes responsible for producing beta globin chains. Each person inherits two of these genes, one from each parent. Unlike the alpha form, this one is usually linked to genetic mutations rather than gene deletions.
If only one gene is affected, the individual may experience a mild condition with little or no symptoms. When both genes are affected, the condition becomes more serious and may require ongoing medical care, including regular blood support and monitoring.
Rare Related Conditions
There are also less common variations within this group of disorders. Some affect multiple types of globin chains and can influence hemoglobin production in different ways. In certain cases, the body may continue producing a different form of hemoglobin that is usually active during early life. This can sometimes reduce the severity of symptoms when combined with other genetic changes.
Comparison Overview
| Type |
Cause |
Severity |
Common Effects |
| Alpha form |
Missing or altered alpha chain genes |
Mild to severe |
Fatigue, anemia, enlarged spleen |
| Beta form |
Mutations in beta chain genes |
Mild to severe |
Weakness, anemia, slow growth |
| Severe alpha form |
Multiple gene loss |
Moderate to severe |
Bone changes, severe anemia |
| Severe beta form |
Both genes affected |
Severe |
Requires regular treatment |
| Rare variations |
Mixed genetic changes |
Mild to moderate |
Higher fetal hemoglobin levels |
| Fetal hemoglobin condition |
Genetic variation |
Usually mild |
Often no symptoms |
Key Points to Remember
- The condition is mainly divided into two major genetic forms
- Severity depends on how many genes are affected
- One form is usually caused by missing genes, while the other is due to gene changes
- Rare variations may sometimes reduce symptom severity
- Early detection and awareness are very important for proper care and prevention
Subtypes and Severity: From Carriers to Severe Disease
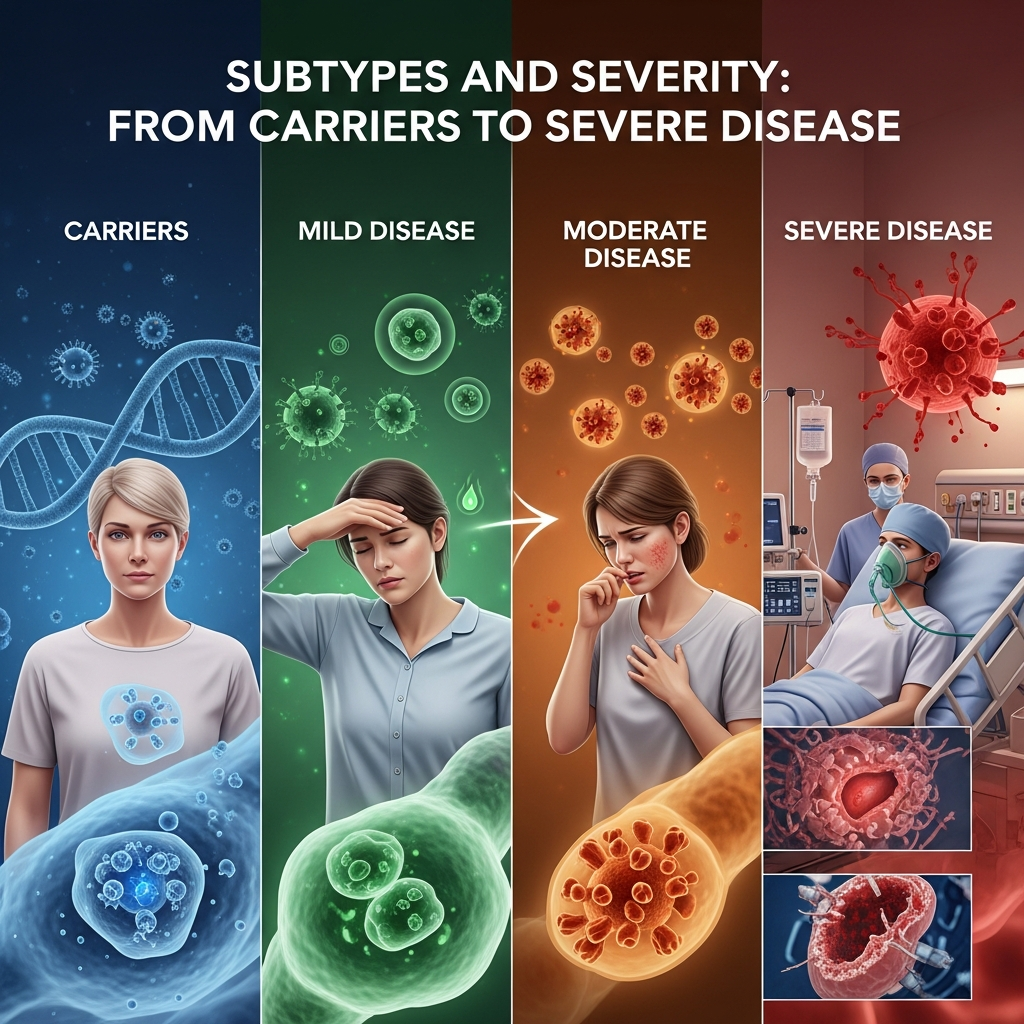 The different types of thalassemia exist on a wide clinical spectrum, ranging from completely asymptomatic carriers to life-threatening conditions. Understanding these variations is essential because the severity of the disease depends not only on whether a person has alpha thalassemia or beta thalassemia, but also on how many genes are affected and how they impact hemoglobin production.
The different types of thalassemia exist on a wide clinical spectrum, ranging from completely asymptomatic carriers to life-threatening conditions. Understanding these variations is essential because the severity of the disease depends not only on whether a person has alpha thalassemia or beta thalassemia, but also on how many genes are affected and how they impact hemoglobin production.
Silent Carriers and Trait (Minor)
At the mildest end of the spectrum are individuals known as silent carriers or those with thalassemia trait (minor). These individuals inherit only one affected gene and usually do not experience serious health problems. In both alpha thalassemia and beta thalassemia, carriers may show very mild symptoms such as slight fatigue or pale skin, and routine blood tests often reveal smaller-than-normal red blood cells.
Although treatment is rarely required, identifying carriers is extremely important. Without proper awareness, two carriers can pass the condition to their child, increasing the risk of severe forms of the disease. This is why genetic counseling and carrier screening play a key role in preventing severe types of thalassemia.
Thalassemia Intermedia
Thalassemia intermedia represents a moderate form of the disorder and falls between minor and major in severity. Individuals with this subtype produce some functional hemoglobin, but not enough to maintain normal health. This can occur in both alpha thalassemia and beta thalassemia, depending on the genetic mutations involved.
Patients with intermedia may experience symptoms such as moderate anemia, delayed growth, bone deformities, fatigue, and an enlarged spleen. Unlike severe cases, they may not require regular transfusions, but they might need occasional blood transfusions during periods of stress, illness, or pregnancy. Long-term monitoring is essential to manage complications and maintain quality of life.
Thalassemia Major (Cooley’s Anemia)
Thalassemia major is the most severe form among the types of thalassemia and is most commonly associated with beta thalassemia major. Babies born with this condition often appear healthy at birth because fetal hemoglobin temporarily supports oxygen transport. However, within the first two years of life, symptoms begin to appear as the body fails to produce sufficient healthy adult hemoglobin.
Severe anemia, poor growth, bone deformities, and organ enlargement are common signs. Without regular blood transfusions and advanced medical care, this condition can be fatal. Even with treatment, patients require lifelong management, including iron chelation therapy to prevent iron overload caused by frequent transfusions.
Diagnosis and Screening
Early and accurate diagnosis is crucial for managing the different types of thalassemia effectively. Because mild forms of alpha thalassemia and beta thalassemia can resemble iron-deficiency anemia, specialized tests are needed to confirm the condition.
The diagnostic process usually begins with a Complete Blood Count (CBC), which evaluates hemoglobin levels and red blood cell size. If abnormalities are detected, further testing is required.
A hemoglobin electrophoresis test is then performed to identify and measure different types of hemoglobin in the blood. This test helps distinguish between various types of thalassemia by analyzing the proportion of normal and abnormal hemoglobin.
For a definitive diagnosis, genetic testing is the most reliable method. It identifies specific mutations or deletions in the genes responsible for alpha thalassemia and beta thalassemia. This is especially important for determining disease severity and planning appropriate treatment.
Importance of Screening and Prevention
Screening plays a vital role in reducing the burden of severe types of thalassemia, especially in high-risk regions. Premarital screening and prenatal testing allow couples to understand their carrier status and make informed decisions.
Early detection not only improves patient outcomes but also helps prevent the transmission of severe forms of the disorder to future generations. Increasing awareness about screening programs is one of the most effective strategies in controlling thalassemia globally.
Management and Treatment Approaches
 Although there is currently no universally accessible cure for all types of thalassemia, modern medical advancements have significantly improved both life expectancy and quality of life for patients. Treatment strategies vary depending on whether a person has alpha thalassemia or beta thalassemia, as well as the severity of the condition.
Although there is currently no universally accessible cure for all types of thalassemia, modern medical advancements have significantly improved both life expectancy and quality of life for patients. Treatment strategies vary depending on whether a person has alpha thalassemia or beta thalassemia, as well as the severity of the condition.
For individuals with moderate to severe forms, regular blood transfusions remain the cornerstone of treatment. These transfusions supply healthy red blood cells, helping to reduce symptoms of anemia such as fatigue, weakness, and delayed growth. However, repeated transfusions can lead to iron overload, a serious complication where excess iron accumulates in vital organs like the heart, liver, and endocrine system.
To manage this condition, patients require iron chelation therapy. This involves medications that bind to excess iron and help remove it from the body through urine or stool. Proper iron control is essential for long-term survival and reducing organ damage in severe types of thalassemia.
For selected patients, especially those with compatible donors, a bone marrow or stem cell transplant offers a potential cure. This procedure replaces defective blood-forming stem cells with healthy ones, allowing the body to produce normal hemoglobin. While this treatment can be life-saving, it is complex, expensive, and carries significant medical risks, making it suitable only for carefully selected cases.
The future of treatment is highly promising. Advances in gene therapy and gene-editing technologies such as CRISPR are being studied to directly correct the genetic mutations responsible for alpha thalassemia and beta thalassemia. Researchers are also exploring ways to reactivate fetal hemoglobin production, which can naturally compensate for defective adult hemoglobin.
Living with Thalassemia
Living with chronic types of thalassemia requires long-term physical, emotional, and psychological adaptation. For individuals with severe forms, daily life often revolves around hospital visits, transfusion schedules, and medication routines.
A well-balanced lifestyle plays a crucial role in disease management. Patients are generally advised to avoid iron supplements unless specifically prescribed, as iron overload is already a major concern. Maintaining a nutritious diet, staying hydrated, and engaging in light to moderate physical activity can help improve overall well-being.
Preventing infections is also extremely important, especially for patients with weakened immunity due to frequent transfusions or enlarged spleen. Regular vaccinations and timely medical check-ups are essential for maintaining health stability.
Equally important is mental and emotional support. Living with alpha thalassemia or beta thalassemia can sometimes lead to stress, anxiety, or feelings of isolation. Joining support groups, both online and offline, helps patients and families share experiences, gain emotional strength, and learn practical coping strategies. A strong support system significantly improves the overall quality of life for those affected by different types of thalassemia.
Moving Forward with Thalassemia Knowledge
Thalassemia is a complex inherited blood disorder that requires deep understanding, early detection, and long-term medical care. By learning about the condition—from silent carrier states and mild forms to more severe variations—patients and families can take a more active and informed role in managing health.
Understanding how this condition affects hemoglobin production helps individuals recognize the importance of early screening, accurate diagnosis, and proper treatment planning. Awareness is especially important in regions where the disorder is more common, as it can significantly reduce the risk of passing severe forms to future generations.
Advances in modern medicine have transformed severe cases from life-threatening childhood illnesses into manageable chronic conditions. With regular blood transfusions, medication to control iron levels, and improved monitoring systems, many patients are now able to live longer and better-quality lives than before.
Even more promising is the future of treatment. Ongoing research in gene therapy, stem cell science, and genetic editing continues to bring hope for long-term solutions. These innovations aim to address the root cause of the disorder rather than only managing symptoms.
If you have a family history of blood disorders or are planning to start a family, it is strongly recommended to consult a healthcare provider or genetic counselor. Screening and early awareness remain the most powerful tools in prevention. By taking proactive steps today, families can significantly reduce the impact of this condition in future generations.
Frequently Asked Questions
1. What are the main types of this blood disorder?
The condition is mainly divided into two primary forms, which affect different parts of hemoglobin and vary in severity.
2. What is the alpha form?
This is an inherited condition caused by reduced or missing production of alpha globin chains, leading to varying levels of anemia.
3. What is the beta form?
This occurs when beta globin chain production is reduced or absent, resulting in anemia that can range from mild to severe.
4. What is a carrier or minor form?
A carrier state means a person has one altered gene but usually shows no or only very mild symptoms.
5. What is the severe form?
The most serious type usually appears early in life and requires regular medical treatment and ongoing care.
6. What is Hemoglobin H condition?
This is a moderate to severe form caused by the loss of multiple alpha globin genes, leading to significant anemia.
7. Can this condition be cured?
A full cure is currently possible only in some cases through advanced medical procedures, while research continues for better treatments.
8. How is it diagnosed?
Diagnosis is done through blood tests and genetic analysis to check hemoglobin levels and gene mutations.
9. Is it inherited?
Yes, it is passed from parents to children through genes.
10. Can carriers have children safely?
Yes, but if both parents carry the gene, there is a risk of having a child with a more severe form, so medical guidance is recommended.
Conclusion
This is a group of inherited blood conditions that vary widely in severity, from mild carrier states to serious lifelong illness. Understanding these differences is important for early detection, proper care, and prevention of complications.
Milder forms may not cause major health problems, but severe cases often require ongoing medical treatment such as blood transfusions and careful monitoring. Medical advances have greatly improved outcomes, and new therapies continue to offer hope for better management in the future.
Most importantly, awareness, early testing, and informed medical advice play a key role in reducing risks and helping families make better health decisions for the future.
 The different types of thalassemia exist on a wide clinical spectrum, ranging from completely asymptomatic carriers to life-threatening conditions. Understanding these variations is essential because the severity of the disease depends not only on whether a person has alpha thalassemia or beta thalassemia, but also on how many genes are affected and how they impact hemoglobin production.
The different types of thalassemia exist on a wide clinical spectrum, ranging from completely asymptomatic carriers to life-threatening conditions. Understanding these variations is essential because the severity of the disease depends not only on whether a person has alpha thalassemia or beta thalassemia, but also on how many genes are affected and how they impact hemoglobin production. Although there is currently no universally accessible cure for all types of thalassemia, modern medical advancements have significantly improved both life expectancy and quality of life for patients. Treatment strategies vary depending on whether a person has alpha thalassemia or beta thalassemia, as well as the severity of the condition.
Although there is currently no universally accessible cure for all types of thalassemia, modern medical advancements have significantly improved both life expectancy and quality of life for patients. Treatment strategies vary depending on whether a person has alpha thalassemia or beta thalassemia, as well as the severity of the condition.


 Medical professionals classify this disorder based on which part of hemoglobin is affected. The main forms arise from problems in the production of globin chains. Along with the common categories, there are also rare variations that can influence how the condition appears and how severe it becomes.
Medical professionals classify this disorder based on which part of hemoglobin is affected. The main forms arise from problems in the production of globin chains. Along with the common categories, there are also rare variations that can influence how the condition appears and how severe it becomes.